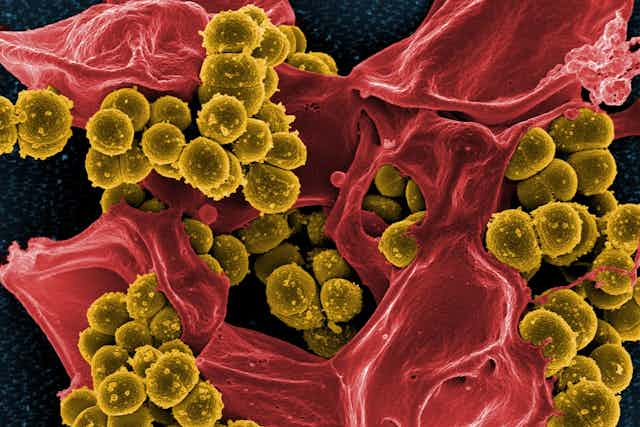
With the world’s attention on COVID-19, I believe that now is the time to talk about another pandemic that’s been happening right under our noses: antimicrobial resistance (AMR).
When infections caused by bacteria, parasites, viruses or fungi stop responding to the medicines designed to treat them, that’s AMR. Resistance builds over time through overexposure to antimicrobial drugs, such as antibiotics, or disinfectants. With ineffective treatments, these infections persist in the body and ultimately spread to others.
A major public health and economic risk
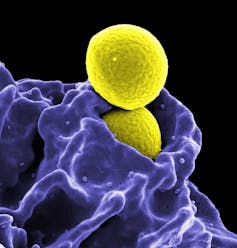
AMR is a slower-moving pandemic than COVID-19, but one that is worsening every day. A recent report by the Council of Canadian Academies said that in 2018, more than a quarter of all infections in Canada were resistant to first-line drugs. In that one year alone, 5,400 people died as a direct result of resistant infections.
Drug-resistant infections lead to longer hospital stays and potentially greater complications. Doctors might need to use alternative medicines with more side effects. These issues cost the Canadian health-care system 1.4 billion dollars, and this will only increase.
The United Nations, the World Health Organization and even the World Bank recognize AMR as a public health and economic disaster waiting to happen. In 2016, United Kingdom economist Jim O’Neill and his team published a report stating that if we do not address the growing threat of AMR, by 2050 more people will die from drug-resistant infections than from cancer.
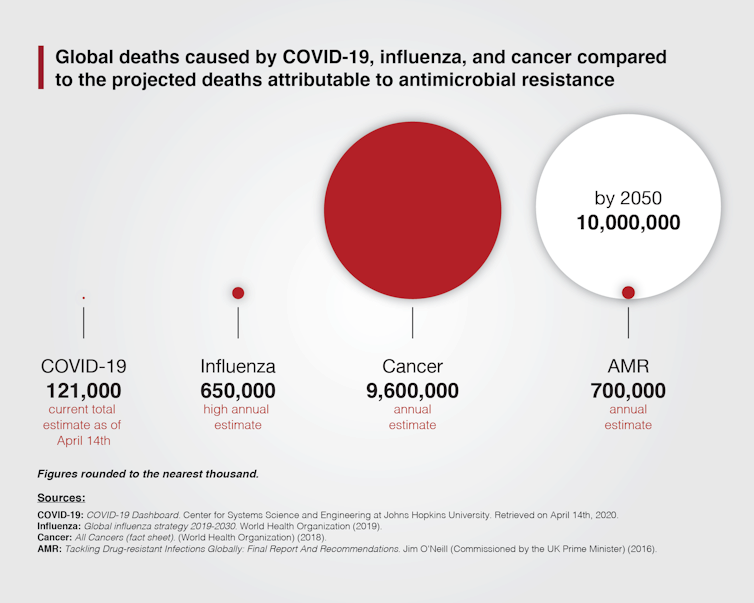
If left unsolved, AMR will cost the health-care system trillions of dollars and, more importantly, it will cost millions of people their lives.
Lessons from SARS-CoV-2
We can learn from COVID-19. The current pandemic shows that despite all of our medical advances, we remain incredibly vulnerable to infections for which we have no therapies. However, it shows that if sufficiently motivated, we can make huge changes in short timeframes.
While there is inspiring work being done in different parts of the world to address the issues surrounding AMR — including here at McMaster University’s Institute for Infectious Disease Research, where my group is based — there is a long road ahead of us.

Despite significant efforts to educate policymakers and the public about the AMR crisis and offer possible solutions, it remains low on the priority list for many jurisdictions. On top of that, research on AMR is woefully underfunded compared to other areas of medicine, such as cancer and cardiac disease.
Another major hurdle for the AMR response is loss of interest by big pharmaceutical companies. The need for expensive clinical trials and the risk of AMR rendering their products useless after a few years mean it’s challenging for them to recover their investment into antibiotic research and development.
Fortunately, antibiotics are only one strategy for fighting bacterial infections. Another common and highly successful approach is vaccination (think about routine childhood immunizations against diphtheria and Haemophilus influenzae), but vaccines are also challenging to develop and deliver in the face of a growing hesitancy movement. Novel treatments such as immune boosters, therapeutic antibodies or natural predators of bacteria called bacteriophages all show promise but are still in the early days of development.
Antibacterial products contribute to AMR
While the key players in the global response to AMR undoubtedly include researchers, food producers, policymakers and health-care professionals, the truth is every single person has a role to play.

One thing we can all do to help combat the spread of AMR is to use regular — not “antibacterial” — soap. Good old-fashioned regular soap is antibacterial and antiviral; it dissolves the greasy membranes that surround bacteria and viruses such as SARS-CoV-2, killing them.
Conversely, antibacterial soaps usually contain additional chemicals that don’t add much in the way of hygiene, but can activate a microorganism’s efflux pumps. The pumps force disinfectants out before they can cause harm (picture someone bailing water out of a leaky boat so it doesn’t sink). They increase the ability of bacteria to fend off multiple types of toxic compounds, including antibiotics, and hasten the spread of AMR.
While COVID-19 in its own right is indeed terrifying, its implications for the future of AMR might be even worse. Widespread use of antibacterial soaps and disinfectants aside, early studies out of China show that almost all severely ill COVID-19 patients were given antibiotics (sometimes multiple antibiotics) to prevent or treat the secondary bacterial infections to which many ultimately succumbed. Unfortunately, the more antibiotics we use, the more we select for AMR.
But I choose to be an optimist. I hope that COVID-19 is a learning experience. I hope it will open the eyes of many to the life-altering power of microbes. I hope it teaches us that we need better (and faster) surveillance infrastructure for outbreaks. I hope it highlights the need for the rapid development, approval and scale up of effective diagnostics and new therapies.
To me, these steps would be encouraging progress in the global response to AMR.