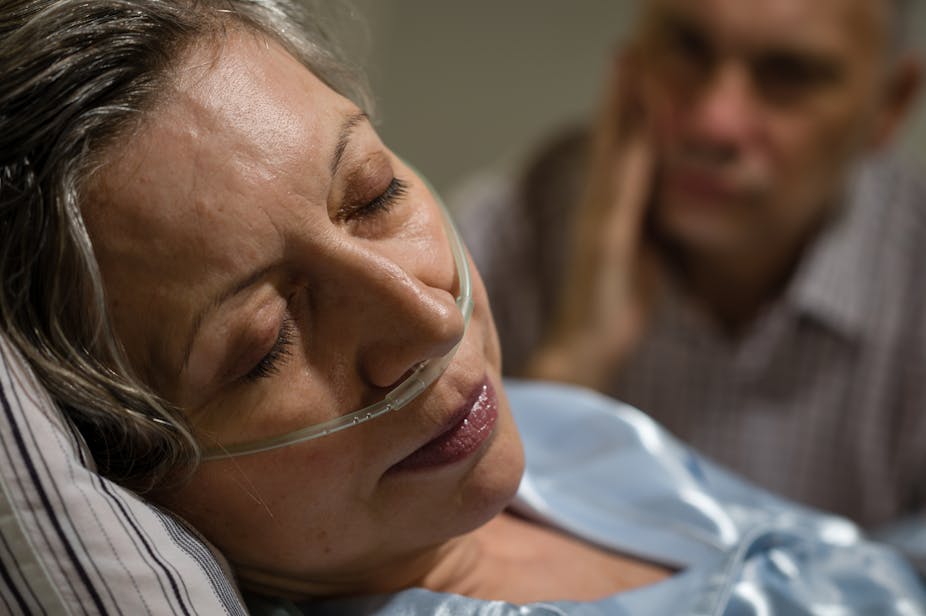
My mother, Sheila Kitzinger, died last month, with good symptom management and with as much choice and control as possible. Her written “Advance Decision” helped ensure that her wishes were followed and she died at home, cared for by her family.
Her experience contrasts starkly with that of my sister, Polly Kitzinger, who was severely brain injured in a car crash six years ago. Polly was subject to a series of life-sustaining interventions (while she was first unconscious and then minimally conscious) that we, her family, believe she would have refused if she had been able.

My sister’s wishes were not recorded in a written Advance Decision. This meant that it was not possible to ensure that her own passionately expressed prior views were respected.
Whatever one’s own individual, family or cultural beliefs, a key question for us all is: “How can we ensure good care, including respect for our values, when we are at our most vulnerable – on the cusp between life and death?”
Dying matters
My family experiences underline my support for “Dying Matters Awareness Week”, which starts today. It also informs my professional involvement in a new cross-university initiative on: “Dying with reduced agency”. This brings together expertise from the universities of Cardiff, Bristol, Bath and Exeter (GW4) to increase understanding of end-of-life issues.
Our key focus is on the end-of-life experiences of people whose ability to make, or enact, their own decisions has been compromised by, for example, dementia, brain injury or chronic conditions of advanced old age.
This is an increasingly important area of work. The ability of modern medicine to heal the body now exceeds its ability to save or restore the mind. The average age at death – and the number of older people dying – is dramatically increasing. But end-of-life care strategies have been led by cancer-related palliative care which often assume an autonomous individual freely choosing to live out a fairly predictable end-of-life process.
A series of scandals in hospitals and care homes reveals a failure to enable good deaths for many and a top-down approach in which patients, families and ground level staff struggle to be heard.
People with reduced agency are vulnerable to both under-treatment and over-treatment. This arises because of poor support and assumptions about their “quality of life” or simply because they are subject to decision-making that prioritises the goals of others.
Professional care providers can impose their own values on their patients. And organisations have institutional cultures, financial considerations, policies and strategies for managing risk that may cut across individual’s wishes.

Family members may find it difficult to represent relatives because they may not know their what their relative would want. And if they do, it might conflict with their own hopes and fears. My own research found that family members can also feel sidelined or silenced by clinicians.
In the UK, “next of kin” have no legal decision-making powers for other adults. However strongly a person believes that their family member would, for example, not want to be sustained in a long-term vegetative or minimally conscious state, they are not able to refuse life-sustaining treatment on their relative’s behalf. The only exception is if they have been formally appointed, in advance, as the person’s lasting power of attorney for health and welfare, with specific rights to make such decisions.
How we care for people with reduced agency is a complex and increasingly significant question. Radical new thinking is required to inform policy and practice. The GW4 initiative will include hosting an arts event and conference later this year and we are planning a major cohort study to examine people’s experiences at the end of life (and the views of their family and professional carers).
Systemic change is needed
We will be examining the significance of the place of care (for example: home, hospice and hospital), the diagnosis (such as dementia or acquired brain injury), and the way in which decisions are made. It is already clear, for example, that there have been failures to implement the Mental Capacity Act 2005, which was designed to “empower and protect” people who lacked capacity to make some of their own decisions.
The 2014 House of Lords post-legislative scrutiny committee found that “prevailing cultures of paternalism (in health) and risk-aversion (in social care) have prevented the Act from becoming widely known or embedded. The empowering ethos has not been delivered”.
Systemic change is desperately needed. Meanwhile, each of us can try to protect ourselves and those around us by having honest conversations about death, recording our wishes in a legally binding Advance Decision or registering someone we trust as our lasting power of attorney for health and welfare.
Many of us would rather not think about the end of life. But unless we do so, we risk having much worse deaths than necessary, and leaving family and friends burdened with guilt and regrets about the way we died.