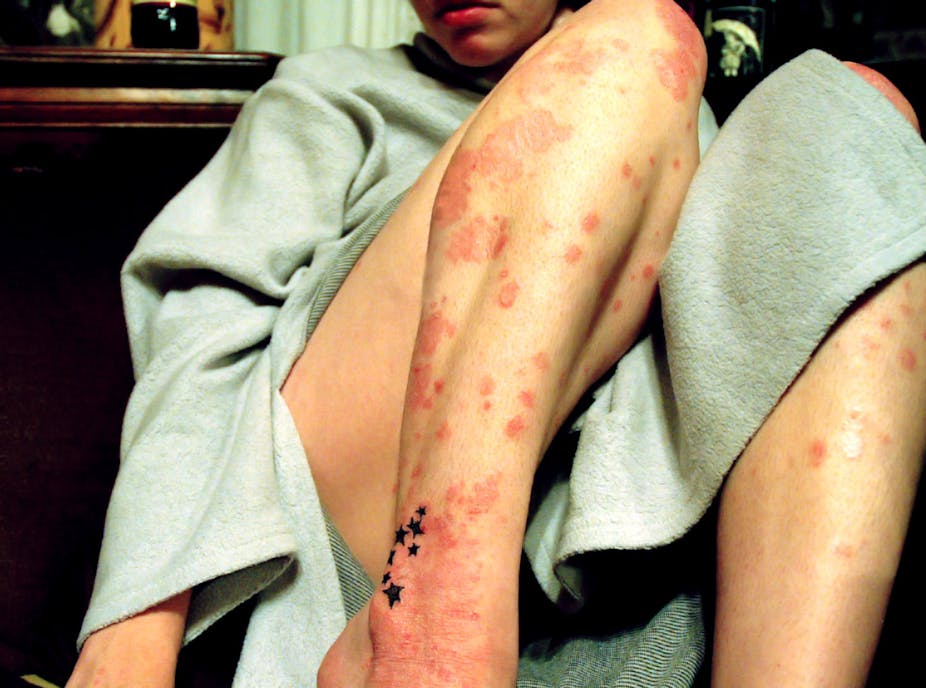
Psoriasis is an inflammatory disease of the skin that affects around 2% of the Australian population. That’s enough people to fill the Melbourne Cricket Ground each of the five days of Boxing day test match.
Psoriasis produces angry red scaly plaques on the elbows, knees and elsewhere; severe dandruff on the scalp; nail discoloration and soreness; and inflammatory arthritis of the joints.
The biblical description of “lepra” is now thought to actually be psoriasis rather than leprosy. At that time, affected individuals were stigmatised and cast out from their communities. Some would argue this remains unchanged today as many affected people feel like lepers.
Causes and symptoms
Psoriasis is hereditary; over 30% of affected people can identify a first-degree relative with psoriasis. Research has also identified a number of susceptibility genes, which, when mutated, increase the risk of psoriasis.
Known triggers include certain drugs such as lithium, and antimalarial and antihypertensive medication, but there is no recognised dietary trigger. The mechanism by which these agents trigger psoriasis is not yet understood.
Skin trauma and surgery can cause psoriasis to seed into the wound; when someone with psoriasis has their appendix removed, for instance, and a new patch of psoriasis appears in their appendix scar, this is known as the Koebner phenomenon.
Stress has long been thought to aggravate psoriasis. And itchiness is variable, with some people driven to distraction while others live in harmony with their condition.
Psoriasis causes the skin to renew too rapidly, with insufficient time for the individual cells to fully mature. Normally, it takes six weeks for cells that divide at the base of the epidermis – the uppermost layer of the skin – to differentiate, die, and shed off the skin surface. In psoriasis, this process occurs ten times faster and only takes four to five days.
This rapid cell proliferation causes the skin to thicken. It also requires increased blood flow and nutrients to support this rapid cell proliferation. Increased nutritional requirements stimulate new growth of blood vessels into the skin (angiogenesis), which makes the skin red.

The new cells pushed to the surface are not fully mature and rather than shedding one by one, as mature skin cells do, they are still stuck together, producing skin scaliness and flaking.
Treatment options
Traditional treatments apart from tar and dithranol ointments include steroid creams, calcipitriol cream or ointment (a synthetic derivative of vitamin D), sunlight, artificial ultraviolet B treatment, and tablets such as acitretin (an oral retinoid), cyclosporine (a drug to prevent organ transplant rejection), and methotrexate (a chemotherapy agent).
Each of these treatments work well for some people but not all. And cumulative side effects often limit their continued use even among responders.
Recent years have seen a quiet revolution in the treatment of psoriasis. Gone are the messy and smelly tar and dithranol ointments. Molecular biology research has delivered a host of new therapies called biologics.
Biologics are a class of treatments where monoclonal antibodies are manufactured synthetically to target a specific molecule in the chain reaction that produces the skin inflammation seen in psoriasis.
Depending on the biologic agent used, a single injection into the skin repeated either fortnightly, monthly or quarterly can produce complete clearance of even the worst psoriasis within weeks. It can also keep the skin disease at bay.
The first biologic therapies for psoriasis targeted the tumour necrosis factor alpha molecule, a master cytokine. Cytokines are cell signalling molecules involved in the regulation of inflammation. These biologics are also used to treat rheumatoid arthritis, Crohn’s gastrointestinal disease, and other inflammatory diseases of the body.
The next generation of agents targeted interlukin 12 and 23. Interlukins are a class of cytokines initially found in white blood cells, but now known to be produced by and act on a broad range of cells in the body. Newer agents are directed at the interleukin 17 molecule.
The cost of these agents is in the range of A$5,000 to A$30,000 per year. The government subsidises the cost of these medications through the Pharmaceutical Benefits Scheme for only the most severely affected. This creates a unusual paradox for dermatologists: treating mild disease is now more complex than treating severe disease.