Our gut does more than help us digest food; the bacteria that call our intestines home have been implicated in everything from our mental health and sleep, to weight gain and cravings for certain foods. This series examines how far the science has come and whether there’s anything we can do to improve the health of our gut.
We used to think foetuses had no bacteria in their gastrointestinal tract (the gut) until they began to accumulate microbes (bacteria, viruses and other bugs) on their way through their mother’s vagina.
But this theory was challenged when bacteria was found in meconium (the first poo) of premature babies. This, of course, travelled through the gut, accumulating microbes on the way.
What’s clear is that newborns have little (if any) diversity in their microbiota – the collection of bacteria that accumulate in the gut. This increases as they’re exposed to different environments.
The particular makeup of a newborn’s gut microbes is important as it has been shown to affect their risk of developing certain diseases in childhood and adulthood.
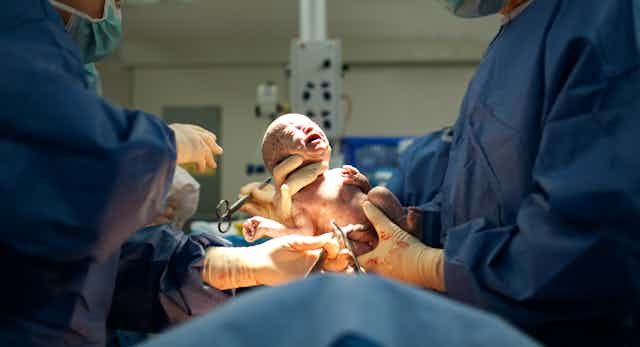
Vaginal or caesarean birth?
The mode of delivery has a big impact on an infant’s microbiota. During natural delivery, the direct contact with the mother’s vaginal and intestinal flora help shape a newborn’s gut bacteria colonisation. Newborns delivered via caesarean section don’t have this direct contact.
One study found that newborns born vaginally were colonised by Lactobacillus whereas caesarean delivery newborns were colonised by a mixture of bacteria typically found on the skin and in hospitals, such as Staphylococcus and Acinetobacter.
These early differences tend to be sustained. One study showed the distinct gut flora of infants born by caesarean delivery persisted at six months after birth. Faecal Clostridia numbers in seven-year-old children born vaginally were found to be significantly higher than in children of the same age born via caesarean.
But we still don’t know how this impacts on children’s health and the risk of disease.
The developing immune system
We’re beginning to realise gut bacteria plays an important role in the growth of infants’ immune systems. One way this could occur is by altering the development of the white blood cells that provide a first-line defence against invading microbes: bugs that make us sick.
Research shows mice born in a germ-free environment have fewer of these white blood cells compared to healthy mice with a normal gut bacteria population. Such mice are also more prone to bacterial infection.
Allergic diseases such as asthma and hay fever appear more often in infants after caesarean delivery than after vaginal delivery.

Children born by caesarean delivery are also significantly more likely to be hospitalised for acute gastroenteritis and to develop coeliac disease.
It’s important to note that not all caesarean deliveries are the same. Some women have caesarean sections after a long labour where her waters have broken. In this case, the infant would be exposed to quite a different microbial environment than a planned caesarean section carried out before her waters have broken.
Breast- or bottle-fed?
Breast-fed newborns have a distinctly different gut microbiome to other newborns. They have higher proportions of the beneficial bacterial species Bifidiobacterium than formula-fed infants. This is likely due to breast milk containing a type of prebiotic that facilitates the growth of bacteria such as as Bifidobacterium.
Interestingly, when breast-fed infants are supplemented with formula feeds, their gut microbiota resembles infants who are exclusively formula-fed.
What does this mean for infants’ risk of developing disease?
A US study has shown that breast-fed babies had a gut microbiome that was richer in genes associated with “virulence”: the ability to fight off antibiotics and toxic compounds. These same babies also developed changes in the genes of their gut immune system that allowed them to better fight off infection.
This suggests that breast milk can promote a healthy crosstalk between the baby’s immune system and the gut microbiome.

Breast-feeding has been shown to reduce the development of necrotising enterocolitis (where parts of the bowel die off) in newborns, allergic and autoimmune diseases in childhood, including coeliac disease, type 1 diabetes and asthma.
Vaginal seeding
What if your child is born via a caesarean section and can’t be breastfed?
Don’t worry, not all such infants will be at a greater risk of developing autoimmune and allergic diseases. A whole host of environmental and genetic factors play a role in determining individual risk.
Vaginal seeding has recently been proposed as one way infants born by caesarean section might gain some of the protective effects of environmental exposure for their gut microbiota.
A proof-of-concept study in 18 infants published earlier this year showed that transferring vaginal fluid to newborns (via a swab across their mouth, nose and face) shortly after delivery by caesarean section can result in microbiome profiles resembling that of infants delivered vaginally.
It is unknown though whether colonisation in this way is partially or fully equivalent to the microbial transfer at labour. We also don’t know whether later health outcomes in these infants are affected by the practice.
Some expert clinicians warn against vaginal seeding because of the potential for unrecognised infections to be transmitted from mother to newborn. There is a risk, for example, of transmitting undiagnosed group B Streptococcus to newborns, given 12 to 15% of women have this organism in vaginal fluid.
Better ways to catch up
For now, it’s more sensible to focus on the practices that have been shown to promote microbiome development in newborns delivered by caesarean. These include delaying the first bath until after 12 hours, placing the newborn on the mother’s skin in the first few minutes after delivery and breastfeeding in the operating room, if permissible.

There has been much effort made in simulating the composition of human milk through adding live gut bacteria (probiotics) as well as non-digestible fibres (prebiotics) to formula. This is thought to assist microbial colonisation and immune responses in formula-fed infants in a similar way to breast feeding.
But hard data is lacking though on whether this approach can lead to a real-life benefit, particularly when it comes to reducing the risk of allergic disorders.
Fortunately, a large clinical research project in New Zealand – the Probiotics in Pregnancy study – will soon be able to answer this question.
Four hundred pregnant women expecting infants at high risk of allergic disease were given either a probiotic Lactobacillus rhamnosus or placebo – 14 to 16 weeks into their pregnancy until they gave birth, or for six months after if they breast-fed.
The researchers will then check if the infant develops allergies such as eczema. The results will be available before too long and may be instrumental in helping to shape health policy.
Read the other articles in our Gut series here.