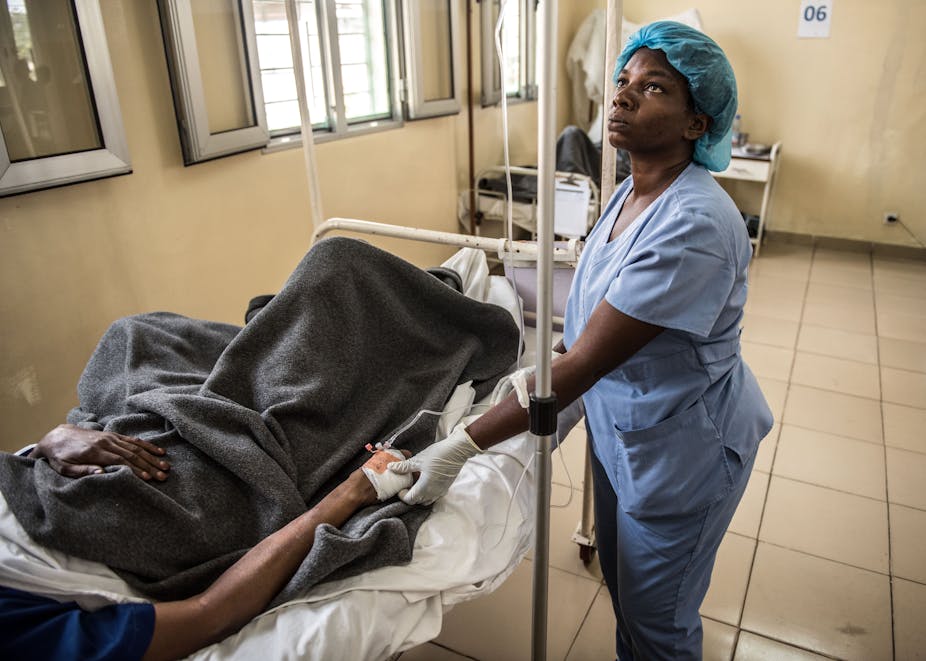
In 2016 I conducted in-depth interviews with patients at a 42-bed AIDS unit run by Médecins Sans Frontières in Centre Hospitalier Kabinda in Kinshasa, as well as caregivers and health staff. My research, which has not yet been published, uncovered the complex, often heartbreaking web of challenges people face living with HIV in the Democratic Republic of Congo (DRC). Nearly 570 000 people live with the disease, which is highly stigmatised. In 2016, the unit treated 2500 AIDS patients. At least 30% arrived so severely ill they died after admission.
Seeing people dying of advanced HIV, commonly referred to as AIDS, was routine at the hospital where I was conducting research. As I noted in one of my diary entries from October 2016:
The hospital register lists the weight of patients on admission: many weigh less than 40 kilograms, some less than 30. One patient in her thirties jokingly lifts her hospital gown and laughs as she shows me the nappy she’s wearing. Another is wheeled into the ward unconscious, wrapped in can only be described as a space blanket. Others are wheeled out of the same door they used when they arrived. But this time, they are covered in white sheets and followed by wailing relatives.
Why do people wait so long before being tested or treated for HIV? Why do those diagnosed stop taking their treatment and wait until they are on the verge of death before seeking medical care?
There are no easy answers. My interviews with health care workers, patients and their caregivers revealed a tangled web of personal, community and health centre barriers that prevented people from seeking clinical care.
I was told people don’t go to health centres when they first become sick due to high costs, lack of knowledge and information about HIV, religious beliefs and, above all, because of stigma.
It’s frustrating to still be writing about HIV-related stigma in 2017. Stigma – and the discrimination that accompanies it – have been common themes in HIV since I began working in the field as an anthropologist in the late 1990s. Unfortunately, it’s no different in Kinshasa today.
Stigma still stands
Stigma is about shame, guilt and fear, and often stems from a lack of knowledge or understanding. It’s stigma that stops people from seeking an HIV diagnosis when they fall ill. People don’t tell those around them they have HIV because they’re afraid of being associated with something believed to be shameful. As a result, they don’t receive the medical and psycho-social support they need.
Caregivers – usually mothers, daughters or sisters of people living with HIV – were frustrated to learn of the diagnosis so late. They felt they could have prevented their relatives from suffering if they had known earlier. Some relatives suspected the person they were caring for was HIV positive, but didn’t want to ask. They were too afraid of hearing the answer they believed meant their loved one would die.
Others didn’t suspect, or preferred not to see, for fear that HIV would bring shame on themselves and their family. One family saw the hospitalisation of their now teenage son as a waste of time, saying he was going to die anyway.
Little information, fewer choices
HIV remains a synonym for death in Kinshasa. There is limited knowledge that someone with HIV can live a normal and healthy life. Unlike South Africa, where billboards proudly display images of people living with HIV, and AIDS activists have had a strong voice for many years, people in Kinshasa aren’t exposed to this kind of information. If they are, it’s on a much smaller scale. HIV remains shrouded in mystery and fear.
Religion is extremely important to people in Kinshasa but it can also be damaging for those living with HIV. The church plays an essential role in people’s everyday lives; it is a source of support, a community, a place of sanctuary. But some churches prevent people from seeking an HIV diagnosis, or from taking their treatment.
I was told of pastors advising people to throw their pills away. Some people had relatives who had disappeared to attend church camps that claimed they could be cured.
Cost
The issue of cost can’t be ignored when looking at why people are hospitalised. I was shocked by MSF staff accounts that they believed health care workers in other facilities were using HIV to make money.
One clinician described health centres as being “like a boutique”. Patients were sent on the equivalent of a medicalised shopping trip. They had to pay for tests, drugs and consultations, while remaining powerless to question the diagnoses -– and shopping lists -– given to them.
Many of these consultations were unnecessary and simply a way for some health care workers to make money. Once someone is diagnosed as HIV positive, their treatment is free. But until that point, they remain in a system they can’t afford. It’s a system with the potential to benefit someone else.
Working together
Together, these individuals, community and health care system barriers create an environment in which it is incredibly difficult to be HIV positive.
Addressing the issues of stigma, cost, limited HIV knowledge and a weak health care system is complex. Potential solutions to the problem of advanced HIV go beyond the walls of MSF facility into the wider community and beyond. There is a need to focus on stigma reduction at a community level, while giving patients, their relatives and health care workers information about HIV.
People testing for HIV and taking ARVs need to know about their treatment and have ongoing counselling. Civil society and community organisations – such as those in South Africa – do not grow overnight. But taking small steps, such as people living with HIV sharing their stories with their communities, and working with local religious groups, can help reduce the stigma and enable people in Kinshasa to access lifesaving treatment they so urgently need.