Australians should now be practising social distancing to slow the spread of SARS-CoV-2, the virus that causes COVID-19.
By creating more space between yourself and others you decrease the risk of person-to-person spread.
Read more: Coronavirus: why should we stay 1.5 metres away from each other?
It’s also essential that confirmed cases, those awaiting test results and people who have recently returned from overseas self-isolate for a minimum of 14 days.
The purpose of these public health measures, and others such as practising good hand hygiene and cough etiquette, is to “flatten the curve” or mitigate the spread of COVID-19.
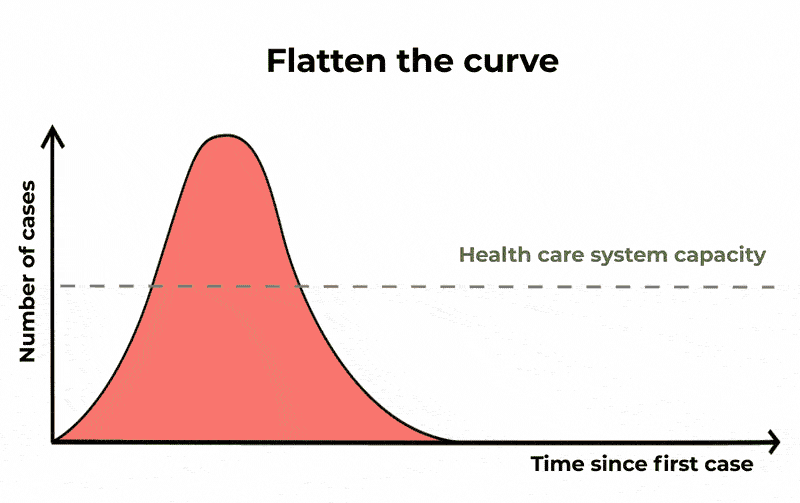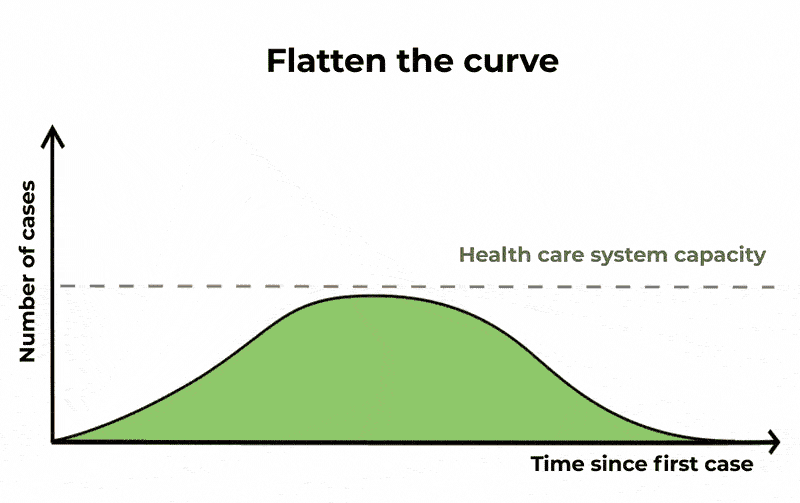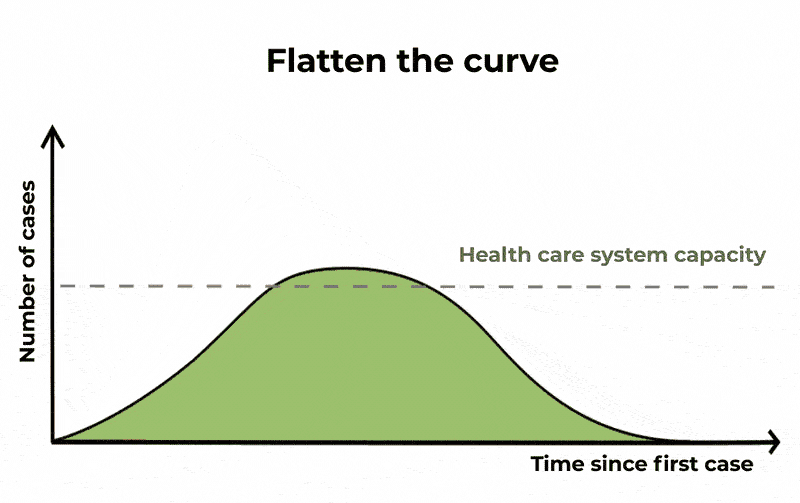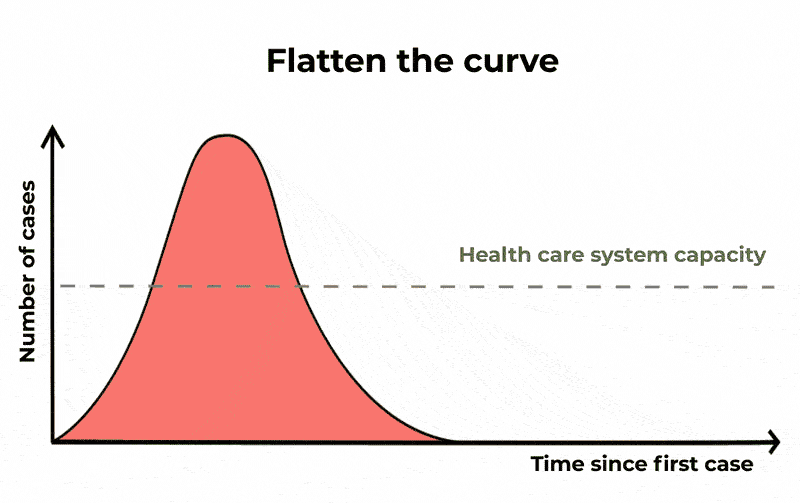
If we don’t slow the spread of the virus and decrease the number of people with it at any given time, our health-care system – and intensive care units in particular – will struggle to cope.
What would uncontrolled spread look like?
As Australian mathematician Joel Miller, from La Trobe University, wrote on The Conversation, without public health interventions, the virus could spread quickly and infect a large proportion of the population:
COVID-19’s observed doubling time has been about four days. That means every four days the number of cases has been roughly double what it was four days prior.
We would calculate it takes about three months for one infection doubling every four days to cause 15 million infections.
After the peak, we expect the total time to drop to be about the same as it took to rise. This gives a crude prediction of six months.
According to data from China, around 5% of people who test positive to COVID-19 will experience severe symptoms and require admission to an intensive care unit (ICU) for around four weeks.
So, three months into the pandemic, without public health measures to control the spread, we could have expected to see 750,000 severe cases requiring admission to ICU in the first three months.
What can our ICUs cope with?
We currently have just over 2,200 ICU beds.
Assuming all ICU beds will be reserved for coronavirus patients, statistician Megan Higgie from James Cook University has estimated that when Australia has 44,580 infected patients, all our ICU beds will be full.
Based on these estimates, Higgie suggests we could run out of ICU beds in early April.
And, of course, chronic conditions and traumatic injuries will persist and people without coronavirus will continue to need intensive care.
What impact can public health measures have?
Modelling published this week by Imperial College London suggests that implementing all available mitigation options, including social distancing and home isolation, could dramatically reduce pressure on ICUs.
The researchers estimate that over a three-month period, these measures could reduce demand for ICU beds by 69%.

But even with the public health measures we have in place to control the spread of COVID-19, the Australian and New Zealand Intensive Care Society suggest the number of ICU beds may have to double to cope with the increased demand.
We don’t just need more beds, we need nurses to staff them
Nurses will need to be mobilised to provide this additional ICU care.
In Australian ICUs, the nurse to patient ratio is 1:1, so one nurse looks after one patient. This is due to the highly complex care needs of these patients who require constant observation, assessment and treatment to remain stable.
We need to identify nurses with critical care qualifications or experience who can be redeployed to address this increased demand.
Nurses who specialise in medical and surgical fields could also be deployed to work in ICUs under supervision.
Recently retired nurses could be called on to rejoin the workforce, as well as those with registration but not practising.
Current leave and future leave from work may need to be limited or cancelled and other health professionals, including defence personnel and student nurses, working under supervision, could be called on to boost the overall nursing workforce.
What else can hospitals do to cope with the increased demand?
As the pandemic evolves, hospitals will experience a triple threat of more patients, reduced numbers of clinical staff as some become infected, and increased illness intensity.
We need to protect front-line health workers from contracting COVID-19 or becoming exhausted, which will also reduce absenteeism.

Hospitals may also need to:
discharge patients from hospital more quickly than previously
postpone admissions for all non-critical procedures
increase the remote and virtual care capabilities, such as telehealth and care hotlines, to treat patients at home
activate alternate care sites such as hotels or small private hospitals for patients requiring low levels of care so we can save large tertiary hospitals for those with greatest need.
This is an unprecedented global public health crisis. Our health systems will be under tremendous pressure over the next several weeks and months, requiring rapid adaptation to meet the needs.
The social distancing measures we adopt now will help us to deliver the best care to patients and each other when we need it.
Read more: Coronavirus will devastate Aboriginal communities if we don't act now

