In India in 2021, an estimated 504,000 people died from tuberculosis, or TB. That’s almost one per minute. More than a quarter of the estimated TB cases worldwide are in India.
In 2018, the UN committed to end the TB epidemic globally by 2030. The “End TB” strategy sought to reduce TB incidence by 80%, deaths by 90%, and eliminate catastrophic costs for TB-affected households.
India announced it would try to eliminate TB in India by 2025, five years ahead of the UN’s target.
However, the first TB survey since the 1950s was recently conducted, and it found rates in the Indian community are much higher than anticipated.
Read more: TB's stronghold in India: A tragedy there, and a grave concern for the rest of the world
What is TB?
Tuberculosis is a disease caused by infection with the bacteria Mycobacterium tuberculosis. It mainly affects the lungs, and the bacteria spreads when an infected person coughs or sneezes.
Some people are infected but do not get any symptoms, which is known as “latent TB”. In others, the infection begins to cause symptoms within weeks or months, which is known as “active TB”.
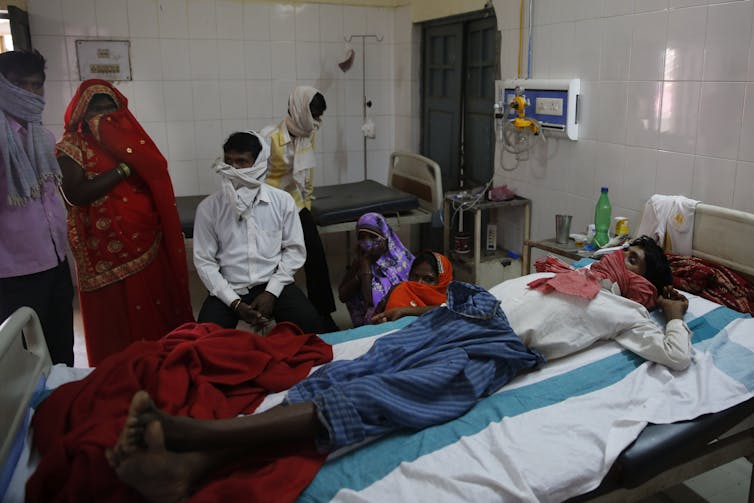
Up to 10% of those with latent TB eventually develop active TB years after the initial infection.
Antibiotics are the mainstay treatment of TB. However, the bacteria has been known to become resistant and find a way to beat these antibiotics. Drug-resistant strains of TB have become a global concern.
Read more: Explainer: what is TB and am I at risk of getting it in Australia?
70 years of TB control in India
When India gained independence in 1947, there were about half a million TB deaths annually and an estimated 2.5 million Indians suffered from active tuberculosis.
In 1948, a TB vaccination program commenced. The BCG vaccine protects against the most severe forms of TB, such as TB meningitis in children, but it doesn’t protect against TB in adults.
Read more: Model of new TB vaccine shows its potential impact and value in South Africa and India
India’s first national survey of TB, conducted from 1955 to 1958, found on average four of every 1,000 people in India had TB.
The National Tuberculosis Institute was established in 1959 and an interdisciplinary group of epidemiologists, tuberculosis specialists, microbiologists, biostatisticians, sociologists, public health nurses and X-ray engineers conducted a series of research studies that culminated in the National Tuberculosis Programme in 1963. The key strategy of the program was to use chemotherapy to treat TB.
What did the most recent survey find?
The results of the most recent national TB survey in India (2019–21) have just been released, and found just over three people per 1,000 had active TB cases. This is not a great improvement on the last survey from the 1950s (four per 1,000) and much higher than the WHO’s 2020 estimate of 1.8 per 1,000.
The highest prevalence was in Delhi, at over five per 1,000. Groups with higher prevalence included the elderly, malnourished, smokers, those with alcohol dependence and diabetics.
Despite the plan to eliminate catastrophic costs due to TB, an estimated 7-32% of TB sufferers and 68% of TB sufferers whose infection is resistant to frontline antibiotics experienced catastrophic costs. Catastrophic costs are said to be incurred when the total costs of treatment exceeds 20% of the annual household income.
What happened to TB during the catastrophic COVID outbreak in India?
The total number of TB patients recorded dropped by 25% in 2020, then rose 19% in 2021.
This probably indicates TB diagnoses were lost in 2020 during the COVID outbreak. Given hospitals were overwhelmed by COVID cases, people with TB symptoms would have been less able to get care, or would have been hesitant about going to hospital for fear of catching COVID. Even the National Institute of Tuberculosis and Respiratory Diseases (NITRD) was converted into a designated COVID Care Centre in May 2021.
One might have thought lockdowns to stop the spread of COVID (which spreads person-to-person) would have seen a decrease in the incidence of TB (which also spreads person-to-person). This effect was certainly seen for infections such as influenza.
We can only speculate as to why TB cases didn’t decrease, but the fact TB was already endemic in India, and the fact lockdowns probably increased overcrowding for socioeconomically disadvantaged households, could have meant TB was able to more effectively spread in crowded households.
This was exacerbated by the healthcare system at time bordering on collapse as resources had to be allocated for COVID cases, and access to diagnostics and treatment were reduced during the lockdown periods.
Read more: As India's COVID crisis worsens, leaders play the blame game while the poor suffer once again
What has to happen now?
India’s National Strategic Plan for Tuberculosis Elimination has described four strategic pillars of “Detect – Treat – Prevent – Build” (DTPB) as the way forward.
Detect refers to early identification of presumptive TB cases, at the first point of care, and prompt diagnosis using high sensitivity diagnostic tests
treatment refers to initiating and sustaining all patients on first-line anti-tuberculosis drug treatment for drug-sensitive TB patients and appropriate antibiotics for drug resistant TB
prevent refers to scaling up air-borne infection control measures at health care facilities, treatment for latent TB infection in contacts of confirmed cases, and addressing social determinants of TB including crowded housing and sanitation
build refers to strengthening and building on the existing health service to prevent and treat TB and positioning TB high on the health and development agenda.
It is looking like we may be too late to reach the 2025 elimination goal. But if we follow these four steps, we might come closer to eliminating TB in India.
Read more: India's ambitious new plan to conquer TB needs cash and commitment