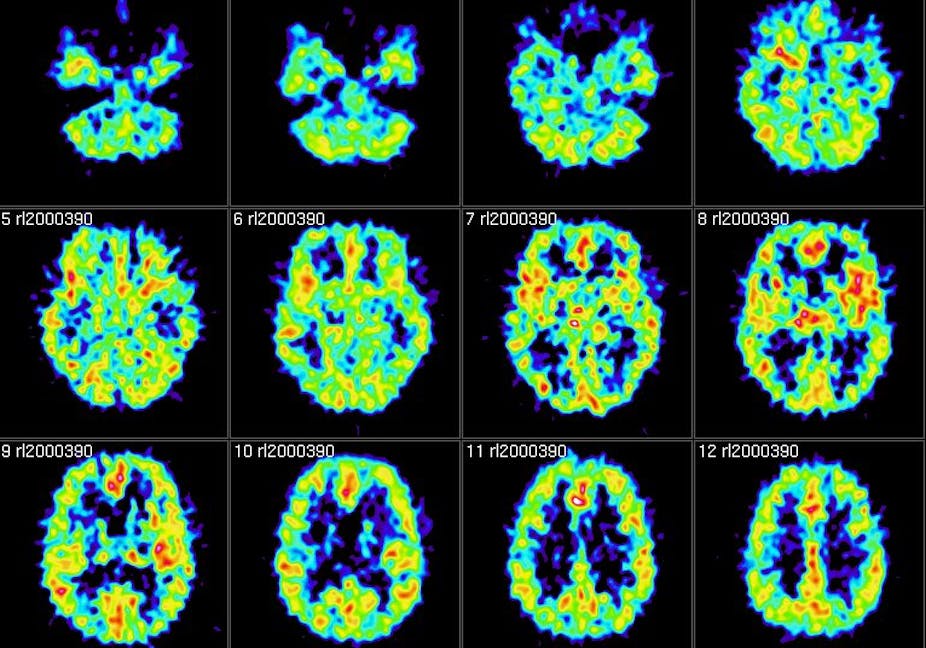
When patients suffer from a brain injury and are unresponsive, we often don’t know whether they have suffered irreversible damage from which they will never recover, or whether the damage is a temporary problem (perhaps even an important part of the brain’s healing process).
In patients with substantial swelling of the brain, working out whether they might wake up is usually done through clinical examination – testing whether they respond to stimuli such as light shone in the eyes – and structural brain imaging. But in many cases the accuracy of predicting the outcome is no better than flipping a coin.
However the results of a promising new study, published in The Lancet, suggest that positron emission tomography (PET), which looks at energy uptake in different parts of the brain, could be particularly good at determining more accurately which of those in a minimally conscious state or suffering from unresponsive wakefulness syndrome (previously described as being in a vegetative state), might regain consciousness.
In some cases it was also able to detect some level of consciousness where CSR-R, the standard behavioural test used by doctors, showed no response.
Define consciousness
Consciousness is a complicated thing, which lies at the interface between science and philosophy. It’s easy to recognise but hard to define. A common definition might be the ability to experience awareness of self and environment, for example. But this is already a circular argument: by using “awareness” to define “consciousness”, aren’t we really just saying “consciousness is the ability to be conscious?”
The situation is further complicated by two other problems. In most diseases where there might be a decreased consciousness, there is also loss of memory. This means we can’t find out if a patient was conscious by asking them later because they might well have been conscious at the time, but the memory has been erased. This is probably quite common during general anaesthesia. The other big problem is that patients may actually be aware of the external world, but are not able to show that they are conscious of it by responding appropriately to stimuli.
The clearest cases of this are people who suffer “locked-in” syndrome – where damage to the lower part of the brain renders them completely paralysed. However this could also – at least sometimes – be the case for people suffering from unresponsive wakefulness syndrome. These people show features of arousal such as eye opening and day/night sleep patterns, but don’t show any behavioural signs of awareness. There are different clinical ways of trying to elicit a response from such patients, but usually you can see that they are vacant, and do not appear to “connect” with anything and anyone in their surroundings.
After this there is a broad classification of minimally conscious states, where people typically have fluctuating periods when they seem to be aware of their surroundings and sometimes even communicate in some way.
Driving consciousness
The exciting part of the new study is that we might be starting to make some progress in understanding the parts of the brain that are necessary for the conscious state, and we can use this to look into the brains of problematic patients to see if these critical regions of the brain are functioning – even if there are no outward signs.
PET looks at the energy uptake of different parts of the brain and if the energy uptake is low, this suggests that area of the brain is not functioning properly. The fMRI technique is different because it looks at changes in oxygenation in different parts of the brain, and if the oxygen level is high it indicates that those areas of the brain are active and working well.
The researchers looked at whether PET and fMRI could distinguish between a vegetative or minimally conscious state in 126 patients with severe brain injury, including four with locked-in syndrome, and a control group that were behaviourally unresponsive but conscious. They then compared the data against the CSR-R behavioural test, which is considered the best test for consciousness.
While the results showed that PET was better at distinguishing a minimally conscious state and was in closer agreement with the CSR-R (the researchers gave it an accuracy of 74% in predicting recovery within a year), in a third of 36 patients that were considered behaviourally unresponsive with CSR-R, the PET showed some level of consciousness. Nine of these later recovered a reasonable level of consciousness, the researchers said.
Brain talk
Our understanding is still at a very early stage, but for consciousness to occur it seems that the critical thing is for widespread parts of the brain to be able to communicate properly with each other – if the network is disrupted, and the information from different parts of the brain can’t reach each other, then the state of unconsciousness prevails.
The problems with the application of the scanning technologies are that they are expensive and tricky to do for sick patients. These patients are also not very common, so it’s difficult to gather large enough numbers to make accurate estimates of the predictive accuracy of the imaging techniques.
However this study is encouraging, as they found a subgroup of patients who appeared clinically unresponsive, but most subsequently went on to recover. They also found there were no recoveries in the subgroup who had low blood flow and metabolism, meaning that PET imaging in combination with the behavioural test could provide a powerful tool for prognosis in cases of vegetative state.
Functional brain imaging, to which both fMRI and PET techniques belong, is a rapidly developing field and these techniques are being continuously developed and refined. And as this is only the start of their clinical applications in this field, it’s a promising sign.