By 2050, drug resistant diseases could be killing more people than cancer, an extra 10m deaths per year. They could also cause a loss to the global output of US$100 trillion dollars – equivalent to a sum greater than the size of the current global economy.
A potential future catastrophe in healthcare, where even routine surgical procedures and easily treated infections become significantly more hazardous, is commonly attributed to the appearance of new strains of antibiotic-resistant bacteria. It is often argued that the answer is more funding for the development of new antibiotics.
What is less commonly recognised is the possibility of a future catastrophe in food production. Modern practice means the extensive use of antibiotics in the farming of fish, poultry and meat. In the US, 70% of all antibiotics enter the food chain.

An arms race against natural selection
Antibiotics are effective against bacteria, just one class of microbe, while the term antimicrobial resistance (AMR) covers the development of resistance in a wider group of bacteria, fungi, viruses and protozoa (such as malaria) to the various measures used to combat them.
The development of new antimicrobial drugs is an arms race against natural selection that cannot be won: when antimicrobials (not just antibiotics) are applied, microbes of all types (not just bacteria) have proven to be adept at developing resistant strains from the survivors. If the drug kills 99.99% of a population of microbes, it is the genetic makeup of the survivors that goes forward to the next generation. To mitigate against potential catastrophes in healthcare and food production, measures over and above the development of new antibiotics have to be undertaken.
These include two key elements. One is infection prevention. If a dangerous microbe never enters the body, no antimicrobial is required. The development of new microbe-resistant materials and products, as well as the development of minimally invasive procedures in hospitals and clinics, improvements in waste disposal and a revolution in cleaning, are some of the measures already being researched.
However, this does not just involve scientists and clinicians. To take just one example, despite all efforts, many in the UK and the US persist in washing their hands lamentably short of the 20 seconds in warm soapy water that experts recommend. We need better leadership to rectify this by implementing advice from those who understand behaviours in workplaces and homes, and we need to invest in science and engineering that makes proper handwashing easy for the public to adopt.
The second element to reducing the use of antimicrobials is the removal of environments that encourage resistant strains to develop, for example in the body of the patient or farm animal, with simple measures such as ensuring a full prescription is taken rather than stopping early when symptoms disappear – a practice that encourages the survival of resistant microbes. Other measures include the invention of sensors to detect infection early and identify the specific microbe present, so that targeted antimicrobials can be used in place of broad-spectrum agents, one example of responsible antimicrobial stewardship.
We must understand how society, climate, land and water resources interact to alter the risk of microbes moving from one host to another. It is a realistic scenario that a resistant strain in a UK hospital might have emerged because of livestock practices half way across the world, where increased flooding, cultural practices, conflict, the movement of money and populations, and the accepted patterns of behaviour, create an environment very different to our own. Conversely, we could find that resistant strains in far-off countries might have their roots in the use of antibiotics in intensive farming in the UK.
The way to do it
The figure below illustrates how the problem extends geographically, and across the workforce and society. The patient in the hospital bed has a reduced risk of infection if the surgeons use a minimally invasive procedure illuminated with lights that deter microbes, and if the surgical instruments, the trays, the rooms, and the tubes that enter the patient (the catheters, nasal drips, endoscopes and so on) are made of materials on which microbes do not readily adhere, and are properly and promptly cleaned (weekend closure of sterile services departments might appear to save costs in the short term but must avoid allowing Friday’s contamination to dry on before washing on Monday).
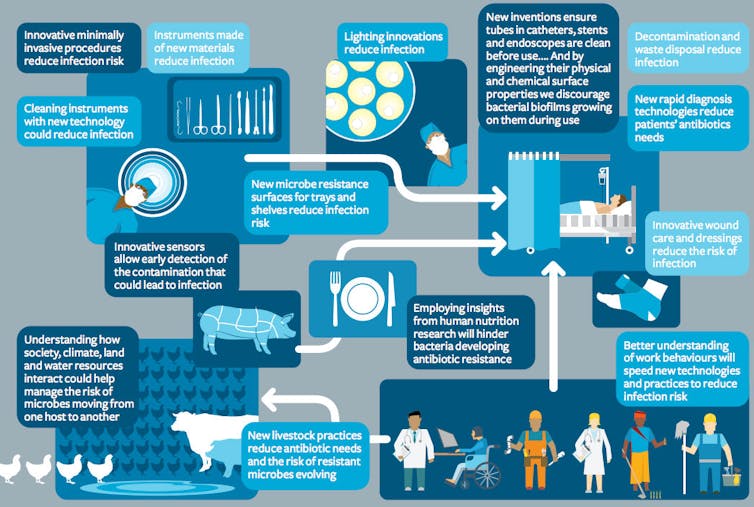
For the patient shown in the figure, wounds can be cleaned and dressed with materials that deter microbes. If infection does occur, it can be promptly targeted with a specific (as opposed to broadspectrum) antimicrobial if it is detected early and rapidly identified (with instruments that feed into a communications hub that alerts the doctor’s phone, which is already becoming equipped with apps containing guidance informed by local susceptibility data).
Treatment of the waste from this patient (solid, fluids and materials contaminated with them) alters the possibility of AMR spreading. Achieving the right hospital environment requires far more than the development of new drugs, and their use by healthcare workers. It goes into the management and maintenance of the hospital, and in to the practices of the people who implement these. New technologies and practices must be designed to ensure that their use will be adopted, which requires understanding design and understanding people.
Indeed, the world outside of the hospital (in the lower half of the figure above) provides an enormous reservoir in which AMR can develop. Analysis and, if necessary, change of our processes and technologies are required in water and waste treatment, and in the production, transport, packaging and retail practices in the food industry.
In many parts of the world, climate change and flooding, war, corruption, politics, received wisdom, traditions and religious practices, and the supply of fuel and money, play a far greater role in food, water, waste treatment, healthcare and the transport of microbes from one host to another, than do the outputs of the drug companies.
The twin potential catastrophes are global, and so are the causes. The solutions lie with scientists and engineers to develop new technologies and embed new practices in the public and workforce; they lie with farmers, plumbers, office workers, water and sewage workers, medical practitioners, food retailers, innovators in business … indeed most of us. And they lie with those who are responsible for shaping behaviour across the world – not just the pharmaceutical companies.