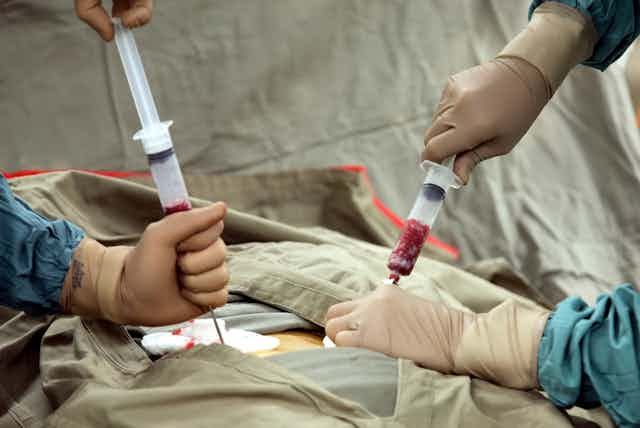
Stem-cell research holds promise for the treatment of a broad range of diseases and conditions, from spinal cord injury to autism. But more work is needed to turn this research into safe and effective therapies.
As a paper published in the journal Cell Stem Cell last week showed, many clinics are skipping this stage. Their websites advertise stem-cell-based procedures despite the lack of evidence for their safety or efficacy. Studies show patients are prepared to pay a high price, at least A$9,000, for these treatments.
Previously, such treatments were available only in developing countries with weak laws or lax enforcement. But last week’s study revealed Australia had among the world’s highest concentration of stem-cell businesses, with websites commonly marketing anti-ageing or skincare therapies. Other developed nations with high numbers of clinics per capita that engage in direct-to-consumer marketing of stem-cell therapies are Ireland, Singapore, Germany, Italy, Japan and the United States.
Desperate patients are therefore at risk of becoming research subjects without the safeguards of a regulated clinical trial. To prevent this, Australia needs to adopt international guidelines that set minimum standards on responsibly translating stem-cell research into clinical practice.
Not therapeutic goods
The range of diseases for which there are proven treatments based on stem cells is minuscule at present. For example, doctors have been extracting blood stem cells through bone-marrow transplants to treat leukaemia for years.
Currently, most stem-cell therapies are experimental. Like a new drug, stem-cell therapies must be evaluated and meet standards before obtaining approval from regulatory bodies to be used to treat humans.
Australia’s Therapeutic Goods Administration (TGA) is the body responsible for ensuring therapeutic goods are safe and fit for their intended purpose. But it excludes autologous therapies, which are those based on the use of a person’s own cells, from being considered “therapeutic”.
These are listed under Section 4 of Excluded Goods, meaning such therapies are exempt from TGA regulation.

Because autologous therapies are based on the cells of the person being treated, there are far fewer moral and ethical questions surrounding their use. The exclusion of these “goods” from TGA regulation was intended to prevent undue regulatory interference. But it inadvertently created a regulatory gap for clinics to conduct untested stem-cell treatments.
Under the present scheme, there are no standards for quality control on how and where the cells are prepared, stored and handled. There is no requirement for monitoring or reporting of adverse events.
International guidelines
The scientific community and advocacy groups have responded to the risks posed by untested stem-cell treatments by formulating guidelines for doctors and clinicians engaged in the clinical application of stem-cell research.
In 2008, the International Society for Stem Cell Research (ISSCR) – an independent, non-profit organisation set up to foster exchange of stem-cell-related information – developed Guidelines for the Clinical Translation of Stem Cells. Updated in May this year, the guidelines build on widely shared principles in research with human subjects, such as the 1949 Nuremberg Code, which holds to principles such as informed consent and absence of coercion.
Developed by a group of researchers from several disciplines – including clinicians, ethicists and regulatory officials from 13 countries – the guidelines provide protocols on the responsible translation of stem-cell research into appropriate applications. The ISSCR also established standards to be observed in yet-to-be-proven therapy.
The guidelines stress informed consent of patients is the cornerstone of clinical studies. Patients must be informed of the source of the cells being used, that stem-cell-derived products have never before been tested in humans and that such interventions may lead to adverse effects, possibly for the lifetime of the patient.
The guidelines state clinicians should share the results of their conducted therapies with other investigators and human-subject research review committees. They should address the risks of stem-cell-based interventions and monitor their patients for long-term health effects with a timely and effective plan for reporting adverse events. Clinicians should seek insurance coverage for the patients to cover any medical complications that might occur.
The guidelines encourage establishing regulatory bodies to monitor researchers and clinicians involved with stem-cell-based products in countries with professional advice and support from ISSCR.
Of course these are merely guidelines – they are not law. Countries have no obligation to follow them. But they can inform the interpretation and development of local laws and guide research practices.
The guidelines are intended to provide a benchmark for clinicians and prompt governments to adopt appropriate regulations. They are a crucial preliminary step in raising the awareness of the international community about these critical issues.
In 2015, the TGA sought community feedback on possible solutions to these issues. The regulator is still considering the submissions received. The next step remains to be seen.