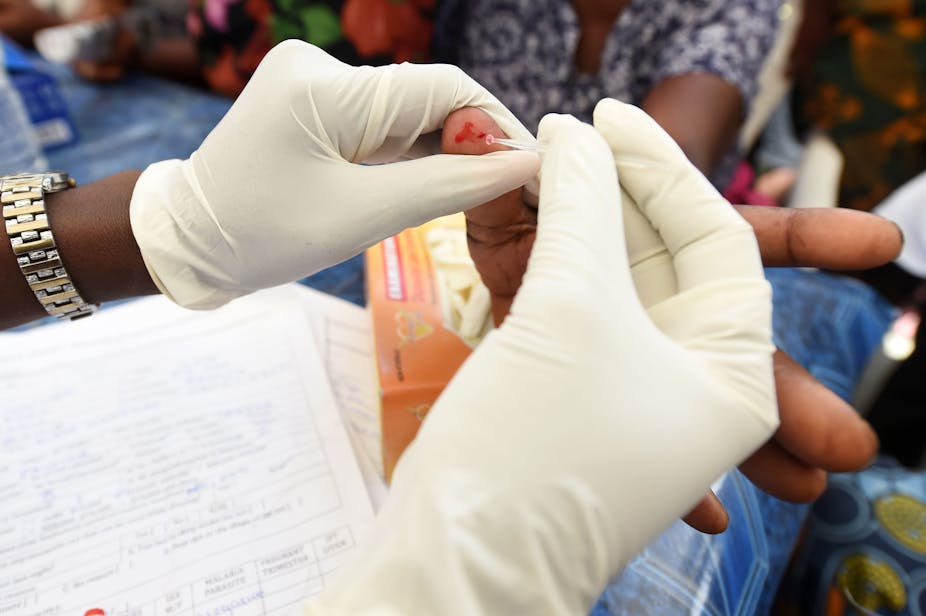
Nigeria accounts for nearly a quarter of deaths from malaria in the world – in 2018 the numbers stood at 95,000. Three of the country’s top malaria researchers reflect on why the numbers remain so high.
What does Nigeria need to do to eliminate malaria?
Olukemi K. Amodu: research and innovate
Malaria remains an important public health hazard globally. It is responsible for high disease and death rates especially among children under five and pregnant women.
The malaria burden in Nigeria is high – 25% of cases globally. The causes include the climate, high transmission potential, socioeconomic development, an overstretched health care system and displaced populations.
Eliminating the disease will take sustained local funding and a strong political commitment at the federal and state levels. This requires a strong recognition of the risk to children and pregnant women. The elimination plan must include focused research and strengthening health systems. It must also be population specific.
It must incorporate World Health Organisation-recommended core interventions. One of these is vector control: protective measures such as insecticide treated materials, spraying to kill mosquito larvae and indoor spraying. The other is diagnostic testing and prompt treatment with effective medicines.
Nigeria needs sustained, interdisciplinary and multi-faceted research. This should be an interplay of basic sciences, clinical epidemiology, field epidemiology, social and behavioural studies. This will ultimately help in studying the differences and diversities in the population. Our federal government must invest more in this type of research.
Malaria prevalence data, clinical epidemiology, parasite diagnostics and rates are important tools for evaluating control efforts. Studies of population biology, genetics and density of the malaria parasite and vector will help find effective diagnostics, new indigenous drugs and new vector control methods.
There must be equal access to health management tools for malaria at all levels. This must embrace educating patent medicine sellers and incorporating knowledge of traditional or herbal medicine practices.
We need to develop new interventions for malaria control suitable for our population.
For example, people say insecticide treated nets are inconvenient, so we also need to develop new ways to use the available protective measures.
Olusegun George Ademowo: beat the mosquitoes
Efforts should be geared towards drastic reduction of contact between humans and mosquitoes. Surveillance is a very important component of malaria elimination.
Environmental management aims to control mosquitoes by removing their breeding sites and larvae. This can be done through clearing bushes around the house and other buildings. It’s important to dispose of broken pots and bottles, fix potholes on our roads and keep gutters clean.
We must also have reliable and affordable diagnostic means for detection of malaria parasites. The most user friendly is the rapid diagnostic test. It detects specific malaria antigens in a person’s blood if they are infected. The most sensitive tests should be identified and made available in health care facilities. They are needed in primary health care and recommended for home use. Expert microscopy should be used to validate the kits periodically.
Artemisinin-based combination drugs are the most acceptable for treatment. They should be made accessible and affordable. Special attention should be given to vulnerable groups: children, pregnant women and non-immune individuals visiting Nigeria from non-malarious countries.
The government must also be willing to eliminate malaria in Nigeria. The Malaria Elimination Programme should be strengthened to evolve relevant home grown means to achieve its goals. The staff must be accountable and dedicated and a monitoring and evaluation system should be put in place.
Segun Isaac Oyedeji: from nets to vaccines
In 1955, the WHO launched the Global Malaria Eradication Programme to eradicate malaria globally.
But not all countries were involved in the programme. After some achieved elimination, its financiers stopped financial support and it stalled. Consequently, the responsibility to eliminate malaria now falls on individual countries.
To eliminate malaria in Nigeria, there must be sincere and sustained commitment by the government, policy makers and citizens. We must be ready to scale up existing malaria control measures and targeted interventions.
Available tools and strategies are currently targeted towards vector control, prompt and accurate diagnosis and effective treatment. These have enormous impact on malaria elimination programmes, succeeding in countries that have eliminated malaria and others at the pre-elimination phase.
The following control measures must be enforced and implemented:
We must ensure that at least 75% of the population use long-lasting insecticidal nets to kill or repel the mosquito that transmits the infection. This would give us “herd-protection” because mosquitoes would find less infected hosts and transmission of the parasite will reduce drastically. Those who have the nets must use them effectively.
We must make sure all pregnant women get treatment.
Government and policy makers may also consider the need for mass drug administration for the entire population at the same time.
Our health systems must be restructured, strengthened and made ready to face the challenges of malaria elimination.
Governments must commit to scale up funding for malaria control, the same way they aggressively pursued COVID-19 prevention and control.
Development of an antimalarial vaccine will also be important for regional malaria elimination and future eradication effort. Getting a vaccine is a global effort and we are at phase III trial currently. Ghana, Kenya, Malawi, Tanzania and Mozambique are involved as study centres or trial sites.