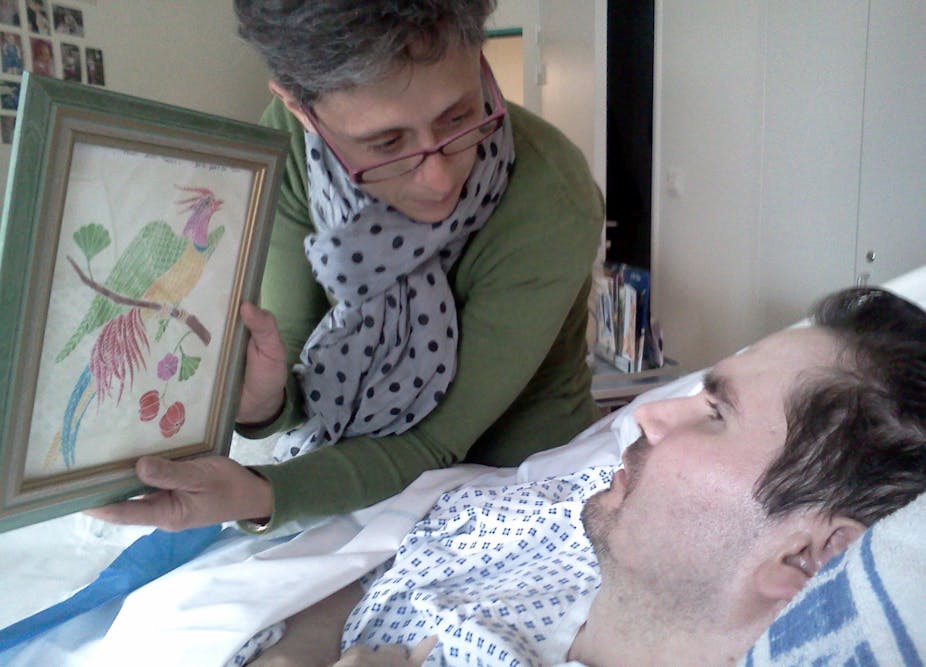
Shortly before Frenchman Vincent Lambert’s life support was due to be removed, doctors at Sebastopol Hospital in Reims, France, were ordered to stop. An appeal court ruled that life support must continue.
Lambert was seriously injured in a motorcycle accident in 2008 and has been diagnosed as being in a persistent vegetative state. Since 2014, his case has been heard many times in French and European courts.
His wife, who is his legal guardian, wishes artificial nutrition and hydration to be stopped and Vincent to be allowed to die. His parents are opposed to this. On Monday, May 20, the parents succeeded in a last-minute legal appeal to stop Vincent’s doctors from withdrawing feeding, pending a review by a UN Committee on the Rights of Persons with Disabilities.
Lambert’s case is the latest example of disputed treatment for adult patients with profound brain injury. The case has obvious parallels with that of Terri Schiavo, in the US who died in 2005 following seven years of legal battles. And there have been other similar high-profile cases over more than 40 years, including Elena Englaro (Italy, court cases 1999-2008), Tony Bland (UK 1993) Nancy Cruzan (US 1988-90) and Karen Ann Quinlan (US 1975-76).

Contrasting responses
There are two contrasting responses to cases like that of Lambert. Some people read about his case and react with horror at the idea of being kept alive against their will in a state where they are completely dependent, unaware of their surroundings and with no apparent prospect of ever recovering.
Other people respond with horror at the idea of stopping feeding and allowing a profoundly disabled man to die, when he does not appear to be suffering and could be sustained in his current condition for months or years.
There are also contrasting ethical arguments. Some people point to the lack of benefit for Vincent in continued life. Because he has no conscious interests, it is not in his best interests to keep him alive, the argument goes. Others contend that his essential human dignity remains despite his profound disability and that his life must be protected “until its natural end”.
The UN Committee for the Rights of Persons with Disabilities might have concern for the rights of the severely disabled to receive life-prolonging medical treatment. But there is a potentially competing right for disabled persons not to receive treatments they would not have wanted and not to have their lives prolonged in states they would have regarded as deeply undesirable.
It can be useful to debate such questions, but the long history of similar cases points to the ongoing challenge of reaching a common view on these issues. Quite simply, we will never all agree on what should happen in such cases. There are opposing reasonable ethical views. The important question is: what should we do in the face of such intractable disagreement?
Our societies are increasingly diverse; we have to accept that people have a range of different values and we should tolerate those differences. That acceptance and tolerance mean that we should allow people to live their lives based on their own ethical views and values, as long as they don’t harm others. It is perfectly acceptable for people to express their views about situations, such as that of Vincent Lambert. But it is not acceptable to impose other people’s views on Lambert’s life.
The only defensible ethical response to reasonable disagreement in cases like that of Vincent Lambert is to make decisions based on his values and wishes. If, as is claimed by Vincent’s wife, Vincent would not have wished to remain alive, then the wishes of his parents, of other doctors or of the Pope, are irrelevant. My views or your views on the matter, likewise, are of no consequence. Only Vincent’s wishes matter. And so life support must stop.