Influenza or flu is one of those dustbin words used by the media and by health professionals to cover the myriad causes of a respiratory infection. The only way to be sure is with laboratory testing of a swab from the nose or throat.
Differentiating between the different viruses is important because some (such as the influenza virus itself) are treatable with antiviral drugs, while many others have no specific therapy.
Some viruses cause trivial disease (like the 100 or so rhinoviruses that cause the “common cold”), whereas others are more severe, particularly in those people whose immune system is compromised. But newspaper reports that drugmakers may have a cure for the common cold rhinovirus are premature because other viruses may be causing the symptoms.
Unfortunately, it’s not always possible to predict who’ll develop severe or even fatal infection. But in principle, general good health is the key. Those who smoke, or are overweight, or elderly, or people whose immunity is suppressed are at the highest risk.
Influenza-like illnesses
In medical parlance, “influenza-like illness” is used to gather together the various symptoms of respiratory virus infections. The clinical features of these infections vary, although they generally include fever, cough or other respiratory symptom, and a feeling of general malaise.
The diagnostic difficulty is that many of the symptoms can be caused by other viruses, some of which are more important in children (such as respiratory syncytial virus or RSV) while others are more severe in the elderly (such as influenza). Some occur mainly in winter outbreaks, others in summer, and others in travellers, who move across seasons.
Respiratory viruses may circulate at the same time: even at the peak of the influenza pandemic in mid-2009 only about half of samples were positive for “swine flu” (influenza A(H1N1)pdm09). Other viruses, such as RSV, adenoviruses and parainfluenza viruses were also commonly detected.
Wheat and chaff
So how can we sort out the really nasty ones from the less virulent viruses? It can’t be done reliably on symptoms alone. Severe symptoms and clinical or chest X-ray evidence of pneumonia are more likely to point to influenza viruses (especially when it’s known that the influenza virus is circulating in the community).
And many of the infections occur in very young children, from whom taking a medical history and examination may be more difficult or unreliable.
The only way to really determine the cause of infections is by laboratory testing of respiratory tract swabs. Newer molecular technologies that detect many individual pathogens means that diagnoses can now be made in about 70% of infections.
Once armed with correct laboratory diagnoses, doctors can decide if treatment is required, and whether infection control procedures to prevent household or workplace spread should be implemented. The likelihood of complications may also be judged at this point. Inappropriate antibiotics can be stopped, reducing antibiotic resistance, adverse effects and costs.
The trouble, though, is that current tests don’t pick up all viruses, results may not be available quickly enough to assist the clinician, and they have a cost.
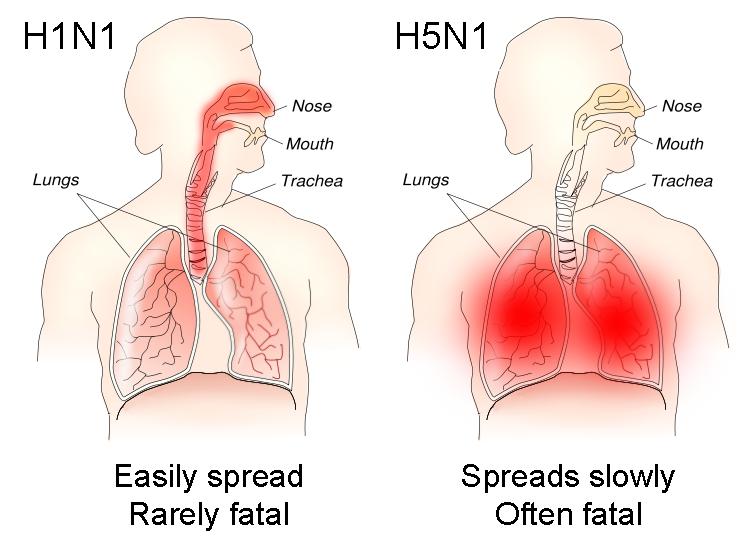
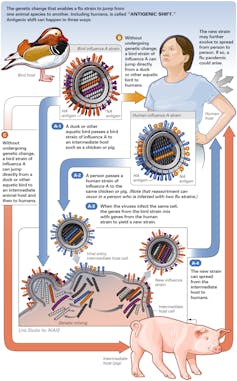
What even further complicates discussion of influenza-like infections is the regular emergence of new viruses. Some of these attract the public eye and media attention, and some may have major medical and economic implications. These include the SARS-coronavirus that appeared in 2003, the “bird flu” (influenza A/H5N1) currently circulating in many countries around the world, and the swine flu pandemic in 2009.
Recent work has shown that many of these organisms come from animals, and that bats may be the original source of many of these viruses.
Economic impact
The impact of influenza-like illnesses is significant, but not always easy to quantify. Healthy adults may have as many as six or eight respiratory tract infections a year, especially if there are young children in the household. The great majority of these are uncomfortable without being serious.
But missing days from work, or having to take time off to care for sick children has a significant economic impact. In the 2009 influenza pandemic, approximately 15% of the population was infected, but only a modest number required hospitalization, intensive care admission or died.
Fortunately, we have a vaccine against influenza, although its efficacy and uptake is not as good as other common vaccines. When targeted to at-risk populations, however, it has a definite public health benefit. But influenza vaccines have no effect on the other respiratory viruses. And vaccines against other common respiratory viruses are not yet available.
Traditional methods of preventing diseases from spreading, such as hand washing (and, perhaps, mask use), remain the mainstay of preventing proliferation of these infections. Spread can be quite rapid, especially in “closed” environments such as nursing homes, military barracks, mass gatherings, boarding schools and so on.
Surveillance, ideally in real time, for both clinical disease and laboratory confirmation of the causative virus, is needed to better understand the nature and frequency of respiratory tract infections. It will also help us detect new strains or viruses as they emerge.

