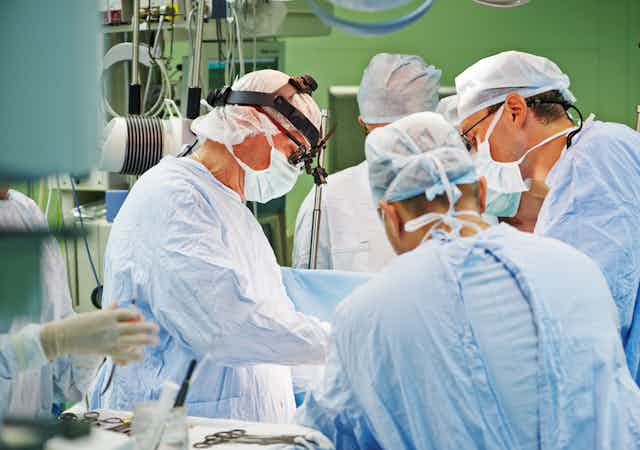
Despite more than 15 years of gender parity in Australian medical education, women remain underrepresented in surgery. The proportion of female surgical trainees is rising, but more slowly than in other specialties.
Of just over 1,000 surgical trainee applications submitted to the Royal Australasian College of Surgeons in 2015, fewer than 300 were from female applicants. In 2015, only 28% of active surgical trainees were female. In comparison, more than 65% of trainees in obstetrics and gynecology were female in 2010.
So why aren’t many female medical graduates choosing surgical careers?
It starts at medical school
Students form some perceptions of specialties even prior to beginning at medical school, yet research shows career aspirations change markedly over the course of medical education. Consistently, a significant factor influencing career choice in medical graduates is gender.
Perceptions of specialties are developed through personal experience and through cultural messages referred to as the “hidden curriculum”. The hidden curriculum consists of the undercurrents of information, not formally part of the medical curriculum, that filter through from peers, patients and lecturers to budding doctors. It is powerful, visible, gendered and discriminatory.
In medicine, these cultural messages perpetuate a distinctly masculine stereotype of a “typical surgeon”. They teach students to anticipate barriers to surgery based on their gender. In one revealing study, both male and female medical students held a perception that surgery is “not a career welcoming to women”.
Although these messages don’t deter the most certain, committed female students from pursuing a career in surgery, students who are less set on a particular specialty are subtly influenced.
In facilitating positive female exposure to surgery and purposefully challenging the stereotypes perpetuated by the hidden curriculum, medical schools, as well as surgical professional bodies, hospitals and government, can play a role in increasing the number of female medical students considering a career in surgery.
Negative experiences of surgical rotations
Medical schools play an important role as the facilitators of the first formal contact of medical students with the surgical profession during hospital-based surgical rotations. This represents a time where gendered perceptions of surgery may be contradicted or reinforced.
Overt discriminatory or sexist comments are the most common predictor of a negative perception of surgery. Rates of gender discrimination, measured in US medical schools, revealed almost ubiquitous experience of gender-based discrimination. During their surgical rotations, 87% of women observed or experienced gender-based discrimination.
The figures for Australian students on surgical rotations are not available. We could assume they have similar experiences.
Students need to be able to report gender discrimination or harassment during clinical rotations and medical schools need to commit to retraining or retrenching teachers who perpetuate gender discrimination.
Female role models
Lack of female role models is a key factor discouraging women from selecting a career in surgery. Surgical programs with higher proportions of female role models in faculty achieve higher numbers of female trainees.
Medical schools need to expose students to a diverse range of surgical role models, as clinical tutors, lecturers or student mentors.
Surgical training programs are renowned for their highly competitive nature, and choosing surgery may be influenced by a student’s perceived preparedness or likelihood of success. Students lacking in research experience, publications or surgical mentors or networks may be less likely to choose highly competitive surgical training positions.
Research productivity among female American academic surgeons initially lags behind male peers. Female surgeons cite lack of time, funding and opportunities for collaboration as barriers to early career research. It is likely gendered patterns of research opportunity and publication are already occurring at the undergraduate student level.
Formalised pathways for research and surgical experience are an alternative strategy to ensure female students gain access to these opportunities which are necessary for a future surgical training application.
Strategies to increase gender equity should be assessed and monitored to make sure they’re working. Transparent reporting of gender data will encourage increased accountability and awareness of ongoing inequalities in surgical education.
Countering cultural messages like those surrounding surgery requires an open commitment by medical schools to improving gender equality in medicine. The message that such disparity is inevitable and intractable needs to be broken down.