
Articles on Health care
Displaying 21 - 40 of 347 articles

A recent study set out to investigate Australia’s long COVID guidelines, services and public health information.

The shortage of family doctors affects not only patients, but the entire health-care system. A strong primary care foundation increases average lifespan, improves overall health and reduces costs.

Cancer screening and other routine primary care can help address inequities if we choose to leave the unfair status quo behind.
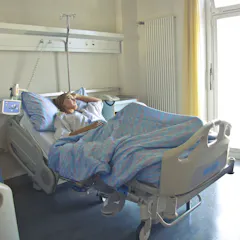
Yes, savings from increased participation in private insurance outweigh the costs the government incurs by subsidising private health insurance rebates. But rebates can be better targeted.

Education has a role to play in addressing the shortage of family doctors. A new program is designed specifically for comprehensive, community-based family practice.

We found rebates don’t do much to encourage older people to sign up for private health insurance.

Each encounter that health-care students have with patients and families helps them understand real-world patient needs. That means all Canadians have a role in educating future health-care providers.

More people are seeking out traditional forms of medicine, from acupuncture to herbal medicines. The WHO is working to develop standards to make these healing practices implementable on a wide scale.

Halfway to the SDGs’ 2030 deadline, countries have made progress, but most are struggling to meet all 17 goals. The US is no exception.

The latest Intergenerational Report shows Australia less old than it was going to be, but poorer. And eventually needing to pay more tax.

Health care has traditionally focused on prescribing medications, with little focus on when to stop them. But pills and potions can add up over time and do more harm than good.

College students who postpone medical care to save money end up paying for it down the line in the form of worse health, a researcher contends.

Increasing awareness of migraine symptoms is critical for those living with undiagnosed migraine, since getting a diagnosis is the first step to receiving appropriate and effective care.

Now is the time to learn from the COVID-19 response through an action-oriented independent inquiry focused on accountability. Reforms to data generation, access and use are essential.

As hip-hop turns 50, an unfortunate reality is that so many of its pioneering artists never live to see much more than 50 years themselves, a professor of hip-hop writes.

The law requires medical test results be made available to patients even before a clinician has reviewed them.

New health technologies raise complex economic, social, environmental and safety concerns. Just as greenwashing tarnished sustainability efforts, ‘responsibility washing’ threatens health innovation.

Tuberculosis is a preventable and curable disease, yet before the pandemic, it killed more people than any other infectious disease.

More than 11 million migrants who lack papers live in the United States, and many of them are ineligible for health coverage.
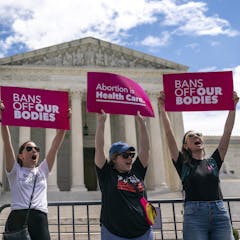
By offering abortion care benefits and policies, employers can serve as a “firewall” to protect against harmful legislation — but only if these benefits are easily accessible and de-stigmatized.
