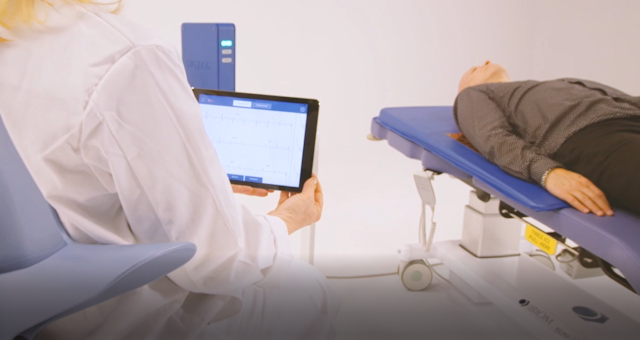
Imagine for a moment an electrocardiograph that’s built into your bed and measures your heart health. No need for a medical professional to be there to attach electrodes to your skin or read the data. This new device might save millions of lives by detecting early signs of heart disease even before any symptoms appear.
Each year, approximately 160,000 Canadians receive a first diagnosis of heart disease. In 2013, half a million Canadians were living with heart disease and were six times more likely to die prematurely. Given the aging population, and the increased risk of recurrence after a first cardiac event, developing new diagnostic tools that make it easier to ensure better heart health is crucial.
We’re part of an engineering research team at the École de technologie supérieure (ÉTS) and Concordia University that is working with an industrial partner to design just such an electrocardiogram (ECG). This promising technology, which could be integrated not only into beds, but also into chairs and other everyday objects, already offers ECG tracings comparable to those obtained by conventional electrodes, and reduces their disadvantages.
The electrocardiogram has to evolve
The technology used to assess cardiac health made great strides over the 20th century, with such breakthroughs as the invention of the modern electrocardiogram by Dutch physician and physicist Willem Einthoven, an accomplishment that earned him the Nobel Prize in Medicine in 1924.
The image of a bedridden patient with electrodes stuck to their chest while their heart activity is being plotted on a millimetre sheet, is a very familiar one to the wider public. Although screens have now replaced paper, the technology itself has changed little over the century since it was invented.
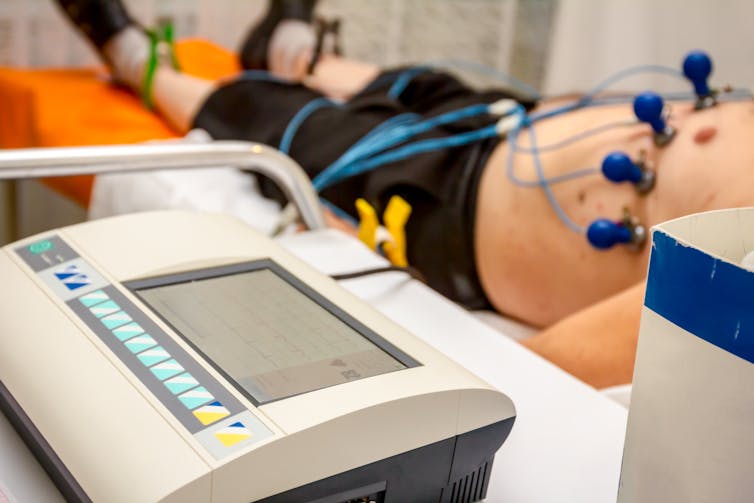
Of course, there are plenty of gadgets today, like smartwatches, that can measure heart rate using optical sensors. While these gadgets maybe be useful for sports training routines, they do not provide an accurate trace of cardiac activity beyond measuring heart rhythm itself.
It might even be time to question the usefulness of electrocardiographs themselves. For example, is it really necessary today to use trained personnel to place electrodes at specific locations on the body? A more efficient method could help clinicians make diagnoses more quickly. And why is it still necessary to use gel, which causes skin irritation for some patients, to apply electrodes?
Recent advances in several technical fields, notably in printable electronics on flexible or textile substrates, are making it possible to design the cardiac health devices of the future. Printable electronics could make it possible for the electronic circuits of the electrodes to be captured directly on textiles or flexible polymers, offering many new possibilities in the process.
For example, the technology we are working on with our industrial partner is based on capacitive sensors that measure the electrical potential — the voltage — created on the skin by cardiac activity. This measurement can be taken through several layers of clothing and does not require attaching any electrodes with gel.
Technical advances at the heart of this new technology
Thanks to rapid advances in printed electronics on flexible substrates, it will soon be possible to create capacitive sensors that can be integrated into a chair or a bed. That will make it possible to take cardiac measurements in real time, not only in a hospital setting, but also while a patient is sleeping or carrying out daily activities.
At the moment, our research efforts are focused on the comfort of these sensors, their robustness under heavy use and how easily they can be cleaned. Once we have overcome these challenges, it will be possible to wear this type of electrocardiograph over long periods of time without experiencing discomfort.
Other challenges are to increase the amplitude of the signals being measured, and to reduce the sensitivity of the sensors to outside interference, especially to the patient’s movements, since the sensors are not attached to their skin. Different approaches to circuit design can both eliminate some of the upstream interference and amplify the useful portion of the signals, while digital signal processing can eliminate the remaining noise.
10 times more efficient with AI
Now let’s imagine combining this technology with artificial intelligence. Algorithms could then accurately determine the positioning of the sensors on the patient. It would also be possible to collect cardiac data at specific locations and specific times of day.
This type of data is extremely valuable for diagnosing cardiac disease. It would be possible to then increase the amount of data being collected by adding sensors and extending the measurement period.

In addition, artificial intelligence will make it possible to diagnosis disease more quickly since the algorithms will have been created specifically to do that. This is the direction we intend to take in our research over the coming years.
Good news for the future
Technologies are advancing so quickly that we believe it will soon be possible to integrate a very comprehensive and inexpensive cardiac diagnostic tool directly into beds. This would be of great benefit to populations at risk for heart disease, such as elderly patients who are losing their autonomy.
It could also be possible some day to perform remote diagnostics with this technology using telemedicine applications. Other biometric sensors for measuring breathing or movement could be added to monitor a person’s overall health and the quality of their sleep.
In the meantime, multidisciplinary collaborations with other research teams will need to work on issues such as data security and privacy.