
Articles on Patient safety
Displaying 1 - 20 of 39 articles

Not all tattoo removal services are licensed, so you’ll have to do some research before booking yourself in. Here’s what to look out for.

But this comes with legal and health risks. Here’s what you need to know before importing medicine for yourself or your immediate family.

Proposed reforms aim to increase public information about previously sanctioned health professionals and to better protect people who complain.

If you’re thinking of a breast augmentation, liposuction, or a face lift, this latest move is designed to provide extra protection. Here’s what you need to know ahead of surgery.

A lack of empathy can be fatal, for both doctors and patients.

Using centuries of indigenous knowledge along with modern healthcare could benefit more people.
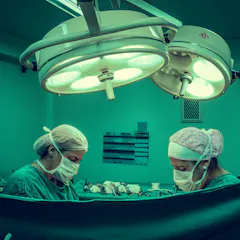
State and territory health ministers have decided to restrict the title ‘surgeon’ to specially trained doctors. It’s a significant change for consumers and doctors.
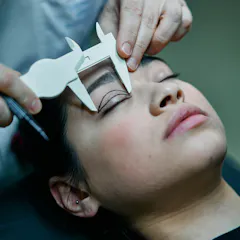
The latest plan is comprehensive, sober, realistic and the product of considerable consultation. But it’s missing a few key issues if we are to adequately protect consumers.

Patient safety incidents were already a leading cause of death in Canada. With that crisis converging with the demands of the COVID-19 pandemic, health care is being pushed to a breaking point.

The UK’s mental health model is broken.

Pausing COVID-19 vaccine rollouts can backfire. There are better ways to manage safety issues while they’re being investigated.

Any COVID-19 vaccine is likely to be given first to higher risk groups before it is given to children. But we still need vaccines that are safe and effective for them too.

The most sustainable and cost-effective solution for protecting patients’ lives is to reduce the causes of human error. Health professionals must be adequately trained to reduce adverse outcomes.

Patients’ wishes must be at the heart of all healthcare decision making.

There are ingredients in your pills other than the one designed to treat your ailments. Those unnamed ingredients can alter how you respond to a medicine or even make you sick.

Organs from gay men or injecting drug users, often rejected for transplants, could safely be used, so long as donors test negative for infections such as HIV, and hepatitis B and C.

New international research shows one in four physiotherapists provide treatments that aren’t based on evidence. These treatments aren’t likely to cause harm, but they might waste patients’ time.

How an implant is designed, tested, regulated and discussed with patients tends to disadvantage women. It’s time that changed.

A botched beauty procedure can be more than just unsightly – it can be dangerous. Here are some things to keep in mind when seeking a skin treatment.

A surprising number of people are catching pneumonia or urinary tract infections in hospital, a new Australian study shows for the first time.
