
Articles sur Health policy
Affichage de 181 à 200 de 370 articles

The AMA has campaigned heavily on the Medicare rebate freeze, pointing out its potential impact on patient access if out-of-pocket costs were to increase.

Labor will lift the rebate freeze from 2017, while under the Coalition, GPs will be paid the same amount for delivering health services in 2020 as they were in 2014. So what does this mean for patients?
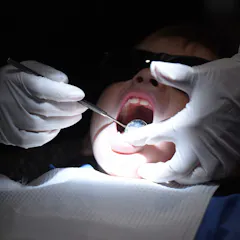
PolicyCheck unpacks the detail and history of the Coalition’s proposed dental health care policy.

We need to focus on keeping people out of hospital by providing better co-ordinated and integrated care.

The Commonwealth wants to partially reverse the cuts it made to public hospital funding in the 2014 budget. But the deal has some unwelcome strings attached.

Fixing the hospital system is not just a matter of more funding. Hospitals need to work smarter, not harder.

There is substantial variation in the safety and quality of care provided in Australian hospitals. The data can tell us why.

Around a quarter of people with private health insurance still choose to use the public system. Why?

Health-care costs are rising, driven by expensive developments in treatments, more demanding populations and rising national wealth. We need to change the financing system to meet this challenge.

Waiting for emergency care, specialist appointments and “elective” procedures is not only inconvenient and frustrating, it can also be painful and detrimental to your health and well-being.
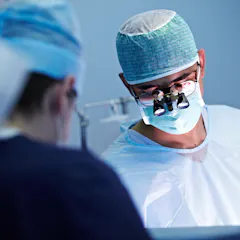
Why is it so difficult to find out exactly how much it’s going to cost to have that suspicious mole removed or to be admitted to hospital for that colonoscopy or hip replacement?
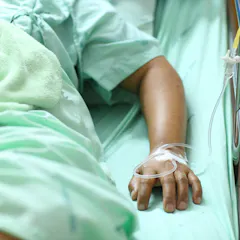
In a time of growing populations, hospitals must guarantee access, ensure quality, minimise the chances of anything going wrong, and do it all within the available budget. So they need to change.

The 5.6% increase amounts to the average family paying about $300 more a year for an average policy.
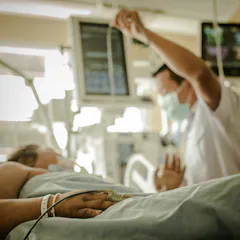
We start 2016 with big challenges for the health system and uncertainty as to how governments will meet them.

Price in health care is a squishy concept. Different words relating to cost – charge, price and out-of-pocket cost – all have different meanings.

This was the year of the health review – mental health care, Medicare, private health insurance, the pharmacy industry … and the list goes on. But how much movement was there on policy?

Britain’s local healthcare system of small time gatekeepers should become stronger networks of powerful providers.

Chronic diseases are responsible for nine out of ten deaths in Australia, and for much of the public health expenditure that’s causing governments so much concern.

When one in six hospitalisations of older patients are due to harm from their medicines, then something is going seriously wrong.

The reforms announced today have the potential to change this appalling situation. But ultimately they should be judged on the outcomes they achieve for patients.
